Kidney Disease Rising as World Kidney Day Marks 20 Years of Global Awareness
Health officials warn that millions may be living with chronic kidney disease as doctors push for earlier screening and stronger prevention measures.
By Chemtai Kirui | Nairobi | March 13, 2026
In a conference hall at the Ministry of Health headquarters in Nairobi on Thursday, the 20th anniversary of World Kidney Day was marked with a message that carried little ceremony: chronic kidney disease is becoming an increasingly serious public health concern for millions of Kenyans.
Health officials estimate that about 3.1 million Kenyans are living with chronic kidney disease (CKD), a long-term condition in which the kidneys gradually lose their ability to filter waste and excess fluids from the blood. Because the illness often progresses silently, many patients only discover it once the damage has become severe.
This year’s World Kidney Day carried the theme “Kidney Health for All: Caring for People, Protecting the Planet,” reflecting a shift in how doctors now understand the disease. Increasingly, researchers say kidney health is shaped not only by conditions such as diabetes and hypertension but also by environmental pressures — from pollution to rising temperatures and water scarcity.
Globally, kidney disease has become a major but often overlooked public health threat. More than 850 million people are estimated to be living with kidney-related illnesses worldwide, and researchers project the condition could become the fifth leading cause of death by 2040 if current trends continue.
Speaking at the Nairobi event, Health Cabinet Secretary Aden Duale said roughly one in every 10 Kenyans now lives with kidney disease — a figure driven by population growth and the rising prevalence of conditions that gradually damage kidney function.
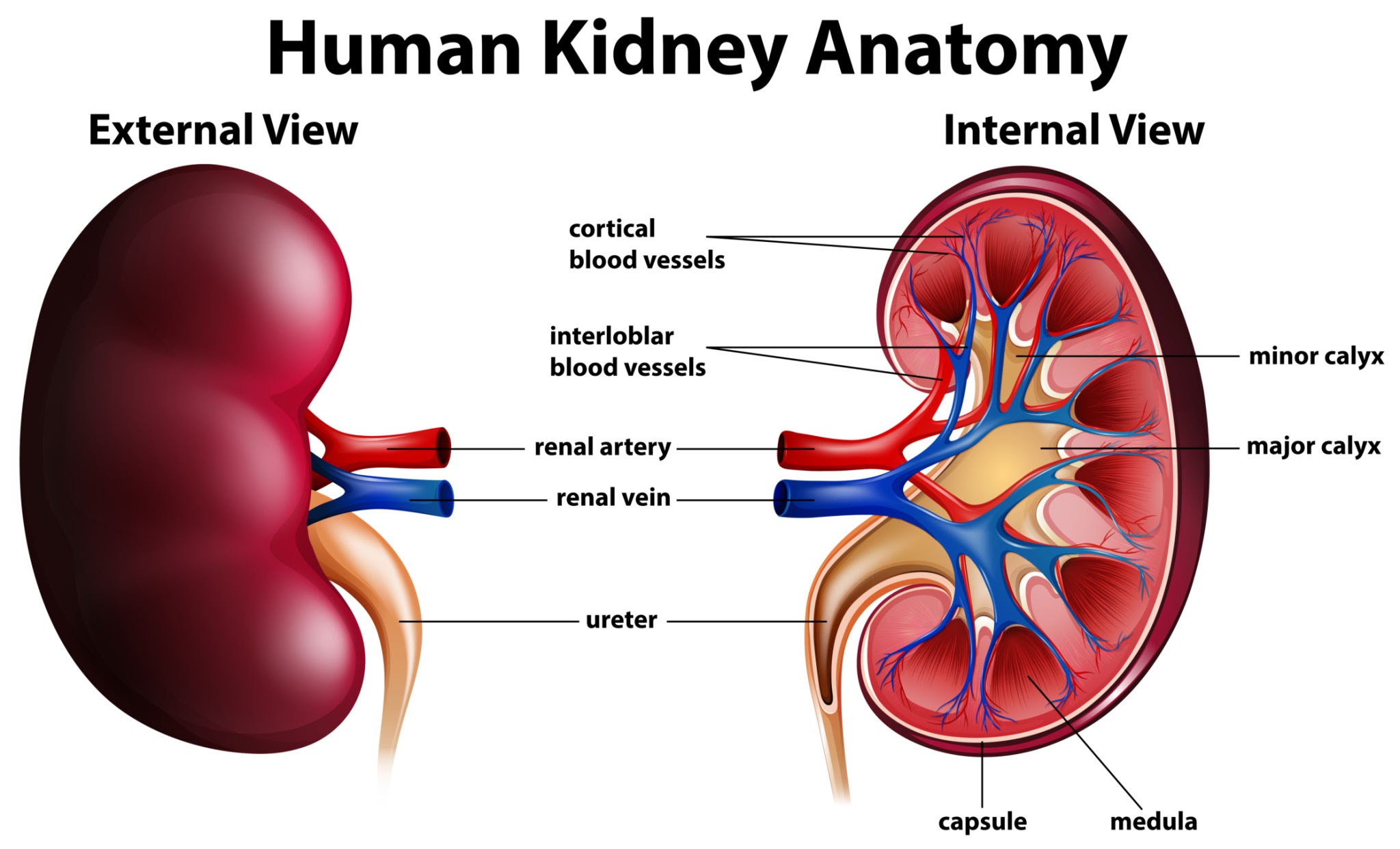
For decades, kidney disease was commonly viewed as an illness associated with old age. But doctors at referral hospitals such as Kenyatta National Hospital say the patient profile is changing. Increasingly, patients arriving at renal clinics are in their 30s and 40s, sometimes younger.
Two conditions are responsible for a large share of these cases: Hypertension and Diabetes. Together they account for a large share of kidney disease globally and are now among the leading causes of kidney failure in the country. Persistently high blood pressure can weaken the delicate blood vessels in the kidneys, while uncontrolled diabetes damages the organs’ filtration system.
But the greatest challenge facing clinicians may not be the causes themselves — it is how late the disease is usually diagnosed.
Because kidneys can lose much of their function before symptoms appear, many patients only seek treatment once the disease has progressed to advanced stages. Doctors say a large proportion of Kenyan patients arrive at hospitals only when they have reached end-stage renal disease, when the kidneys can no longer function without medical intervention.
At that stage, treatment options narrow to dialysis or kidney transplantation.
Dialysis, a process that mechanically removes waste and excess fluids from the blood, has become a lifeline for thousands of patients across the country. Yet it is also one of the most expensive long-term treatments in the healthcare system.
For years, many Kenyan families faced overwhelming financial strain when a relative required dialysis several times each week. Under the previous national insurance framework administered by the National Hospital Insurance Fund, patients often exhausted their annual coverage limits long before the year ended. When that happened, communities frequently organised fundraising drives—known locally as harambees—to cover the cost of life-saving treatment.
The government has attempted to address that gap through a new healthcare financing structure introduced in recent reforms. Under the Social Health Authority and its Social Health Insurance Fund, dialysis sessions at accredited treatment centres are now fully covered.
Even so, the economics of kidney disease remain daunting. A single dialysis session in a private facility can cost between Sh9,500 and Sh16,000. Patients with advanced disease typically require three sessions per week. Kidney transplants, while potentially life-saving, can cost between Sh1.7m and Sh2.5m depending on the complexity of the procedure and postoperative care.
Beyond the surgery itself, transplant recipients must take immunosuppressant drugs for the rest of their lives to prevent organ rejection. These medications can cost tens of thousands of shillings each month, placing additional pressure on families and insurance systems alike.
At the national level, healthcare planners face another challenge: the limited number of specialists able to treat kidney disease. There are fewer than 100 nephrologists serving a population of more than 50 million people in the country. As a result, renal clinics at referral hospitals often face long waiting lists even for routine consultations.
While health officials work to expand treatment capacity, scientists are increasingly focusing on the environmental factors that may be contributing to kidney disease. Researchers have begun documenting clusters of kidney injury among agricultural and outdoor workers in some regions, particularly in hotter and drier areas of the country.
Researchers say the connection is becoming clearer. Prolonged exposure to heat and dehydration can place significant strain on the kidneys, especially for people who perform physically demanding work outdoors. In areas where access to safe drinking water is limited, repeated dehydration can increase the risk of acute kidney injury and kidney stones.
Water quality is another growing concern. Studies from different parts of the world have linked exposure to heavy metals and other contaminants in groundwater to declining kidney function over time. In Kenya, researchers say more data is needed, but early findings suggest that environmental conditions may be shaping patterns of kidney disease in some communities.
Even the treatment of kidney disease carries environmental consequences. A single dialysis session can require more than 100 litres of water, along with significant electricity and disposable medical materials. This has prompted growing interest in “green nephrology,” an emerging field focused on reducing the environmental footprint of renal care through water recycling and more energy-efficient dialysis systems.
For policymakers, the challenge is balancing immediate medical needs with long-term prevention strategies.
The Ministry of Health has recently developed updated national guidelines aimed at strengthening kidney disease screening within primary healthcare services. The goal is to identify patients earlier, before kidney damage becomes irreversible.
Early detection remains the most effective defence. Simple tests—such as blood pressure monitoring and urine analysis—can identify early signs of kidney damage long before symptoms develop. These tests are inexpensive and widely available, yet many people do not undergo them until a serious health problem emerges.
As the banners marking the 20th anniversary of World Kidney Day come down, health officials say the most important work lies ahead. The message from clinicians and patient advocates alike is that kidney disease does not need to remain invisible.
But preventing the silent progression of kidney disease will require more than awareness campaigns. It will depend on routine screening, stronger primary healthcare systems and a broader recognition that kidney health is closely tied to the environment, lifestyles and economic realities shaping everyday life in the country.